I guess I'll just have to ask the chemist to give me 28 tablets instead of 30 tablets because the Discovery scheme is too stupid to allow for convenience. Let's see how this works in 2019. (see note below)
Update Thursday 27th December: I got a call from Discovery after they had read my blog. They have to monitor mow many tablets I have in order to comply with government regulations. I suggested that instead of refusing the claim at the chemist, they should be a little more proactive and send me a note warning me that I already have too much medication on hand and I should delay my next visit until I have used up the meds. That would require just a single extra visit to the chemist to get an extra supply of the 28 day medication. This cycle repeats every 420 days, so a warning would be appropriate at 420-30=390 days, or 420-60=330 days. In my case the refusal was issued at 373 days, which is both inconvenient and impractical.
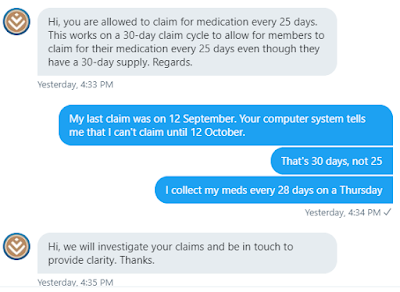
Update Thursday 10th October: Their computers decided to dictate which days I can go to the Chemist. My previous visit on 12 September went without incident. When I arrived on Thursday 10th October, my prescription was rejected. Come back on 12th October, the computer said.
Dear @Discovery_SA you are only allowing me to get my meds every 30 days. How do you suggest I deal with the Pill, which works on a 28 day cycle? Which two days must my wife miss?
— 🇿🇦 Human Being (@donnedwards) October 10, 2019
I sent a direct message with my account number and got the following response:
Update Friday 11th October: The "clarification" came in the form of a patronizing phone call where the Discovery drone repeated that I can collect my medication after 25 days, but I'm not allowed to collect it before 12 October. What kind of contradictory nonsense is that?
Update Tuesday 15th October: I got another "explanation" call from Discovery today. They blame the pharmacist. How convenient. But it gets more confusing. My prescription started on 30 September 11 years ago. So they check my medication over a "year" to make sure I didn't claim more than I should have. How then does a claim get rejected on 10 October, 10 days into the new year? Because they included it in the previous year, of course. The pharmacist allegedly said my 20 day supply was for 30 days, but when we checked it, the script was correct for 20 days. They can't tell me which script was wrong, and they can't fix it either. The pharmacist must fix it. But when I pointed out that if they reverse a claim older than 3 months and then resubmit it, the new claim will be rejected because it is older than 3 months. Catch 22. Basically they have no idea what is going on. Their new motto is: "The computer is always right. We use it to screw the customer."
Update Wednesday 16th October: I got a nice long explanatory email that is extremely short on specifics.
The Medicine and Related Substances Control Act 101 of 1965, has [sic] amended, together with the Good Pharmacy Practice (GPP) Guide published by the South African Pharmacy Council describes appropriate best practice in dispensing scheduled medicines to the public by pharmacists. In applying electronic restrictions on the quantity and frequency of medicines claimable, we are enforcing what we expect to happen routinely in a pharmacy in accordance with regulatory pharmacy and registered medicine use. In this way we also enforce pharmacy risk management on our claims and this serves to protect both members and the Scheme from any fraudulent activities.Personally, I find the implication that I am somehow trying to defraud the scheme to be insulting and offensive. Also, I still have not been told why a claim after 28 days was rejected ("our system will allow you to claim every 23 days instead of waiting for 30 days"), but the same claim after 30 days was not. They also haven't explained which rule I broke: the quarterly or annual rule. And for which period?The law states that not more than 1 month supply of a medication can be provided at a time – these are the “prescribed conditions” that take the interval between prescriptions into consideration as well as the maximum registered dose per days of supply. We electronically enforce monthly prescription refill rules to accommodate the legislation within a reasonable claiming period i.e. 23 or 26 days instead of 30 days.
The onus is still on the pharmacist to ensure that legal prescription refill intervals are enforced. If this is not done, we have additional quarterly and annual validation rules that ensure we do not reimburse in excess of routine allowable prescription filling rules.
For example, the pharmacist can submit 13 fills for 30 tablets in a 12-month cycle and our system will allow you to claim every 23 days instead of waiting for 30 days (4 fills in 90 days). Should there be a discrepancy in which the quantity submitted on a claims doesn’t match the number of days of therapy submitted on system, this might cause the system to reject the claim. However in those instances, the pharmacist can call our Propharmaceutical Benefit Management Department to get clarity on the rejection and check if a possible override can be done
If you have any more questions, please visit www.discovery.co.za to log a query or call us on 0860 99 88 77.
Update Thursday 31st October: I finally got an explanation that makes sense. The explanation of 16 October is just bullshit. What really happens is this:
- An annual claim cycle is 392 days of supply. That's one calendar year plus 27 days. That's 14x28 = 392.
- You can claim early (23 days or more) but they keep a running total of the period for which you claim. This is the "days of therapy" total. If you claim for 20 days, but the chemist lists it as 30 days, you're screwed.
- If I claim every 28 days and claim for 20 days instead of 30 days every 5 months, then I get (4*30+20) = 140 over 5*28 = 140 days. I can do that twice in the year.
- Then I will do another 4 months of 30 days, and end up with 8 extra tablets after 392 days. At which point their system will probably reject my next claim. We'll see.
Once again @Discovery_SA refuses to pay for some of my medication and for my wife. This has been going on for over a year now. #fail https://t.co/Xn03FXyuFn
— 🇿🇦 Human Being (@donnedwards) January 3, 2020
Update Thursday 9rd January 2020: On Wednesday the Social Media team phoned me and put me through to someone in Chronic Medication who had no idea what my query was about and handn't read this blog. I hung up. Then I got an email from discoveryhealthsurveys@discovery.co.za to find out if the query was resolved. I replied and said
The person who called me had no idea what my complaint wasSo a lady from Mujeeb Bray's office (Head of Service) phoned to help. I gave her the short version and she phoned some other department and then phoned me back. I explained to her that their computer system was broken, but she tried to tell me what to do. Each "solution" she offered hasn't worked in the past. That's when I realised that she hadn't read this blog either. At that point I lost it. This is beyond ridiculous.
https://donnedwards.openaccess.co.za/2018/12/discovery-health-doesnt-understand.html
Why is it that everyone at @Discovery_SA Health tries to explain to me why their computer system is right and the customer is an idiot who needs to be trained?https://t.co/Xn03FXyuFn
— 🇿🇦 Human Being (@donnedwards) January 9, 2020
Update Monday 13th January 2020: I phoned Discovery's call centre on 0860 99 88 77 and told them I had run out of the tablets they rejected on 3rd January. What must I do? They contacted the notorious ProPBM department, and asked for the "block" to be lifted for my medication, and then we did the same thing for my wife. ProPBM is a "Pharmacy Benefit Management" system sold by McKesson in the USA. Their crappy system is the one that rejects my claims. What I am supposed to do is ask the pharmacy to call 0860 776 726 and speak to this department whenever a claim is rejected. Discovery lays the entire blame on the shoulders of the pharmacist. How convenient. Next time this happens I will be sending this long tirade to chronicqueries@discovery.co.za because the management of the ProPBM department is too scared of hearing from the public. I'm not surprised, given how pig-headed they are.
Update Tuesday 3rd March 2026: Once again the nonsensical "you can't have 13 scripts in a year" mantra screwed up my visit to the pharmacy. They will give me some medication, but the rest of my wife's meds will only be vailable on 11th March. It's a Wednesday, when I don't have the car. So I have to call a ride to go to get the meds. I would do it over the phone but I'm not sure the pharmacy will get the script right. Today the ProPBM department refused to speak to me, only the pharmacist. They referred me to the Chronic department, knowing full well that they were already closed. Nice try, Discovery!
>



No comments:
Post a Comment